URGENT CARE IN CARMEL, INDIANA
Urgent Care in Carmel, IN — Walk In Today
Physician-Led Urgent Care in Carmel, Indiana · No Appointment Needed · Open 7 Days a Week
Same-day care for illness and injury. On-site X-ray, labs, and treatment in one visit. We work alongside your existing primary care doctor through Epic and MyChart — we are not a PCP, we are the same-day care that keeps your record intact.

URGENT CARE IN CARMEL, INDIANA
Urgent Care in Carmel, IN — Walk In Today
Physician-Led Urgent Care in Carmel, Indiana · No Appointment Needed · Open 7 Days a Week
Same-day care for illness and injury. On-site X-ray, labs, and treatment in one visit. We work alongside your existing primary care doctor through Epic and MyChart — we are not a PCP, we are the same-day care that keeps your record intact.
Same-Day Urgent Care in Carmel, Indiana
Looking for urgent care in Carmel, IN? Monarch Medicine provides fast, physician-led medical care for patients of all ages — no appointment necessary. Whether you are dealing with a sudden illness, an unexpected injury, or need same-day testing, our Carmel urgent care clinic is here to help you feel better today.
Monarch Medicine is an independent, locally-owned urgent care clinic founded by Dr. Lisa Clay, MD. That means shorter wait times, careful evaluation by a Monarch physician, and a clinical team that takes the time to listen. We opened our doors in May 2024 with one mission: provide Carmel families with quality urgent care — without the ER wait or the ER bill.
We are not your primary care doctor — we are the same-day care that works alongside them. Monarch Medicine uses Epic and MyChart, the same systems most local PCPs use. When you see us, your visit notes can be shared with your existing primary care doctor or specialist so your record stays intact.
Our Carmel clinic is located at 90 Executive Drive, Suite A & B — just minutes from Carmel City Center, Clay Terrace, and US-31. We serve patients throughout Hamilton County, including Fishers, Westfield, Noblesville, and Zionsville.
Why Carmel Families Choose Monarch Medicine
Physician-led urgent care you can trust
See a Physician
Every patient is evaluated by an experienced, board-certified physician on our team — not through a non-physician-only visit model.
Independently Owned
Locally owned and physician-led. Decisions about your care are made in this clinic, not in a corporate office.
Minimal Wait Times
Most patients are seen within 15 to 30 minutes. Skip the ER wait and get back to your life faster.
Transparent Pricing
Known in-office costs reviewed before treatment. Self-pay rates published online. LabCorp bills lab work separately.

How Can We Help You Feel Better Today?
- ✓ Walk-Ins Welcome — No Appointment Required
- ✓ Open 7 Days: Mon–Fri 8am–6pm | Sat–Sun 9am–12pm
- ✓ On-Site Digital X-Ray & Lab Testing
- ✓ 5.0 ★ Rated on Google — 170+ Reviews
- ✓ Most Insurance Accepted · Self-Pay Rates Published
Urgent Care Services in Carmel, IN
We treat a wide range of illnesses and injuries for patients of all ages.
Illnesses We Treat
- ✓ Flu, colds & respiratory infections
- ✓ COVID-19 symptoms & testing
- ✓ Strep throat & sore throat
- ✓ Sinus infections & congestion
- ✓ Ear infections
- ✓ Pink eye (conjunctivitis)
- ✓ Urinary tract infections (UTIs)
- ✓ Nausea, vomiting & mild dehydration evaluation
- ✓ Fever evaluation
- ✓ Mild allergic reactions & asthma symptoms without severe breathing distress
- ✓ Headaches & migraines
- ✓ Skin infections & rashes
Injuries We Treat
- ✓ Sprains & strains
- ✓ Minor fractures
- ✓ Cuts & lacerations (stitches)
- ✓ Burns (minor)
- ✓ Sports injuries
- ✓ Workplace injuries
- ✓ Back & neck pain
- ✓ Insect bites & stings
- ✓ Splinter & foreign object removal
- ✓ Animal bites (minor)
On-Site Services
- ✓ Digital X-rays with same-visit physician review
- ✓ Rapid strep, flu, COVID, RSV testing
- ✓ LabCorp blood draws & urinalysis
- ✓ EKG
- ✓ Sports & school physicals (IHSAA)
- ✓ Healthcare student physicals
- ✓ Tdap booster & TB testing
- ✓ Stitches, glue & staples
- ✓ Splinting & crutches
- ✓ Medication given on-site
- ✓ Specialist referrals
Monarch Medicine provides urgent care services for families throughout Carmel, Fishers, Westfield, Zionsville, and Noblesville. From treating illness and injury to on-site diagnostic testing, our physician-led team delivers same-day care without the wait or cost of an emergency room.
Looking for our wellness or compliance programs? See Tdap, TB Testing & Titers, NAD+ Injections, Vital Immunity Boost, or GLP-1 Weight Loss.
WHAT WE DON'T DO — AND WHERE TO GO
We Tell You What We Don't Offer
It is tempting in healthcare to list every possible service. We would rather be clear. We list what we actually do, and we tell you where to go for what we do not offer. Your time matters.
Primary care & annual wellness visits → We are not your PCP. We coordinate with your existing primary care doctor through Epic and MyChart. If you do not have a PCP, IU Health Carmel, Ascension St. Vincent Carmel, and Community Health Network are good places to check for primary care availability.
Emergency conditions (chest pain, stroke symptoms, severe allergic reaction, anaphylaxis, major trauma, severe respiratory distress) → Call 911 or go to the nearest emergency room.
Flu shots, COVID vaccines, MMR, Varicella, Hep B vaccines → CVS, Walgreens, or Kroger pharmacy. Faster and less expensive than urgent care.
Travel vaccines (yellow fever, typhoid, Japanese encephalitis) → IU Health Travel Clinic or Passport Health.
Pediatric well-child immunizations → Your child's pediatrician.
IV fluids, IUD placement or removal, cryotherapy → Your PCP, OB/GYN, or a dedicated specialty clinic.
Other services not listed here → Call us at (317) 804-4203 before you come in. We will tell you honestly whether we can help or where you should go.
If you came in expecting one of these, we want you to know before you make the trip.
FROM DR. CLAY
We Are Not Your PCP. We Are the Same-Day Care That Keeps Your Record Intact.
I have been a physician for nineteen years. In that time I have learned one thing about urgent care: when a clinic tries to be everything, it can lose sight of doing the important things well.
Monarch Medicine is urgent care. We are the place you come when you cannot get into your primary care doctor today and you do not need an emergency room. That is what we do, and we want to do it well.
Here is what makes that work: we use Epic and MyChart, the same systems most primary care offices in central Indiana use. When you see us, your visit notes can flow back to your existing PCP. The labs we draw, the X-rays we take, the medications we prescribe — your doctor can see all of it.
And when your situation needs a specialist's care, we coordinate that referral so the next step is clear — you do not have to figure out where to go next.
If you do not have a primary care doctor yet, we will tell you that finding one matters. We will help you understand what you need today, and we will point you toward the right next step.

DEEPER GUIDES
Looking for Something Specific?
Self-Pay Pricing
Transparent rates for patients without insurance.
Same-Day X-Ray
On-site digital X-ray with radiologist read.
Sports Physicals (IHSAA)
Same-day IHSAA physicals for student athletes.
Healthcare Student Physicals
Tdap, TB testing, titers, and physicals for nursing & allied health programs.
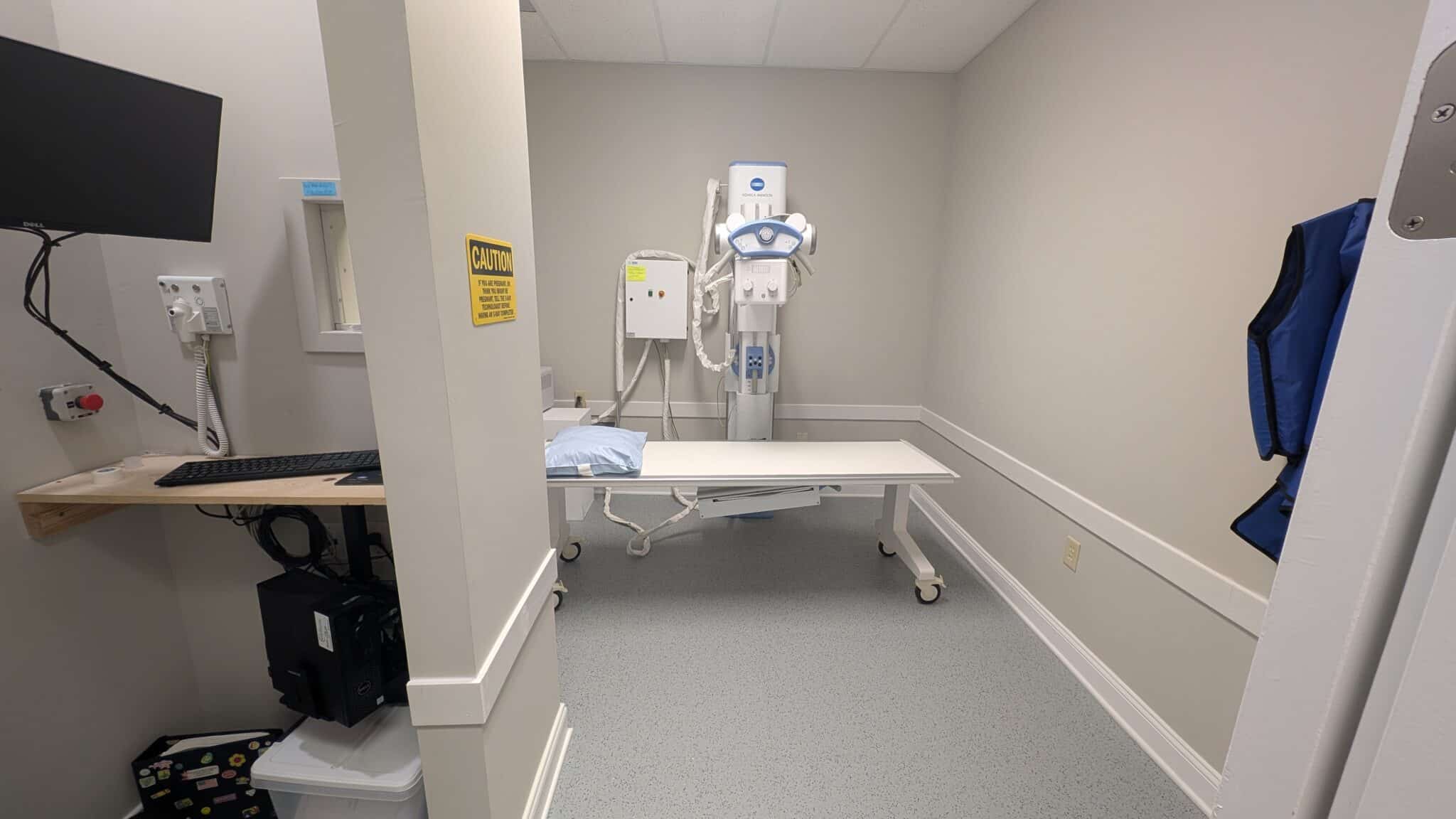
Visit Monarch Medicine Urgent Care Today
Walk-in urgent care in Carmel, Indiana. No appointment necessary. Same-day evaluation, on-site diagnostics, and treatment from a Monarch physician. Serving Carmel, Fishers, Westfield, Zionsville, and Noblesville families seven days a week.
FREQUENTLY ASKED QUESTIONS
Urgent Care in Carmel FAQ
Do I need an appointment for urgent care at Monarch Medicine?
No. Walk in any time during open hours. You can also book online through our MyChart link if you prefer to hold a time.
What are Monarch Medicine's hours?
Monday through Friday, 8am to 6pm. Saturday and Sunday, 9am to 12pm. Open seven days a week.
How long is the wait at Monarch Medicine?
Most patients are seen within 15 to 30 minutes. Wait times can vary during peak illness seasons (winter respiratory illness, fall sports physicals).
Does Monarch Medicine have X-rays?
Yes. We have on-site digital X-ray with same-visit imaging. A Monarch physician reviews your X-ray during your visit, and a radiologist's final read follows after the visit, and timing may vary. See our X-ray page for details.
What insurance does Monarch Medicine accept?
We are in network with Anthem BCBS, United Healthcare, Aetna, Cigna, and Encore/IU Health Plans. We are NOT in network with Medicaid or Humana. Self-pay is also available.
How much does an urgent care visit cost without insurance?
A new patient low-level visit starts at $153.30. An established patient low-level visit starts at $105.70. Costs vary based on testing, imaging, and treatment needed. See our full self-pay pricing.
Does Monarch Medicine see children?
Yes. We provide pediatric urgent care for children, including same-day evaluation for fever, ear infections, strep throat, RSV, COVID, and minor injuries. For very young infants, severe symptoms, well-child visits, or routine immunizations, see your child's pediatrician or go to the ER when appropriate.
How much is a sports physical at Monarch Medicine?
$65.80 self-pay for an IHSAA sports physical. Walk in or schedule online. Forms completed and signed by a Monarch physician during the visit. See our sports physicals page.
What's the difference between urgent care and the emergency room?
Urgent care treats non-life-threatening illness and injury that needs same-day attention — flu, infections, sprains, cuts, minor fractures. The emergency room is for life-threatening conditions: chest pain, stroke symptoms, severe trouble breathing, major trauma, severe allergic reactions. When in doubt, call 911 or go to the ER.
Where is Monarch Medicine located?
90 Executive Drive, Suite A & B, Carmel, IN 46032. Just minutes from Carmel City Center, Clay Terrace, and US-31. Free parking onsite.
WHAT PATIENTS SAY
Read What Carmel Families Say About Monarch
Real reviews from real patients, pulled directly from Google. We have earned a 5.0 rating across more than 170 reviews. Read what your neighbors are saying.
Walk In Today. We're Open and Ready.
Same-day urgent care in Carmel. No appointment needed. Most insurance accepted.
Book An Appointment Call (317) 804-4203
Mon–Fri 8am–6pm · Sat–Sun 9am–12pm
90 Executive Drive, Suite A & B, Carmel, IN 46032
How This Page Is Reviewed
This page was medically reviewed by Dr. Lisa Clay, MD — Founder and Medical Director of Monarch Medicine Urgent Care. Pricing, hours, insurance contracts, and service availability are reviewed regularly because these can change. A Monarch physician reviews your specific care needs and any costs with you before treatment begins. Last reviewed: May 2026.
Medically reviewed by Dr. Lisa Clay, MD — Founder & Medical Director, Monarch Medicine Urgent Care. Last reviewed: May 2026.
Urgent care services at Monarch Medicine Urgent Care are provided by physician-led clinical staff under the supervision of Dr. Lisa Clay, MD. This content is informational and is not a substitute for individual medical advice or care. For life-threatening conditions, call 911 or go to the nearest emergency room. Patients with specific health conditions should discuss their care with a Monarch physician or their primary care provider. Insurance coverage and self-pay rates are accurate as of the page's last review date and may change.
